The human body's immune system plays an essential role in protecting against different infections. When the body encounters a foreign intruder—like a virus—the immune system gets to work to help fight it. Part of this process prepares the immune system to fight the intruder more quickly in the future. However, the immune response meant to offer vital protection sometimes makes the body sicker if exposed to the intruder again. This phenomenon is called antibody-dependent enhancement (ADE).
Notably, despite ongoing reports from experts driving pandemic policy stating there is little to no direct evidence of ADE in SARS-CoV-2 or as a result of COVID-19 vaccines, the potential risk for its occurrence is real and presents a considerable challenge for virus prevention and vaccine development.
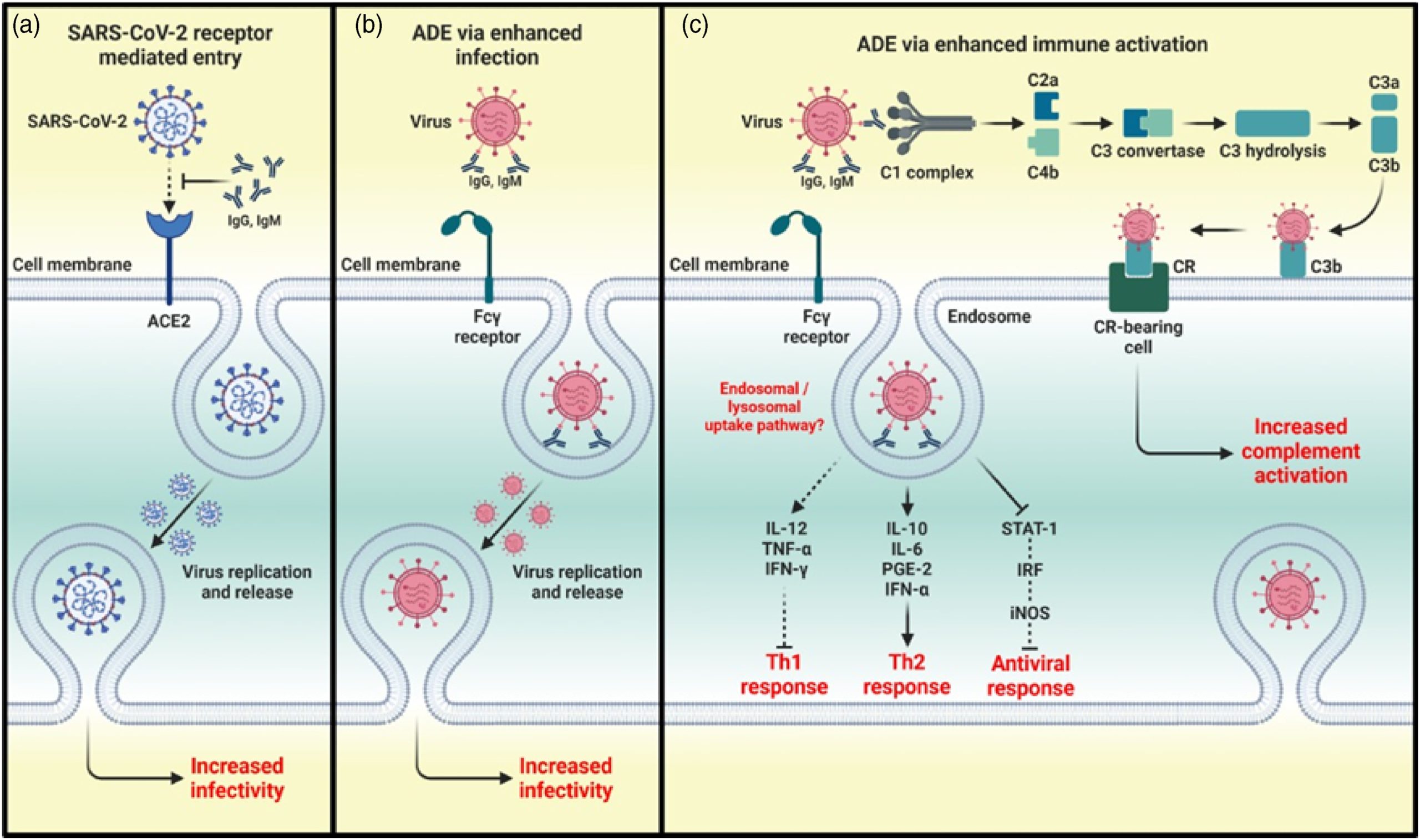 ADE phenomenon. (a) The conventional mechanism of infection by SARS-CoV 2 consists of the binding of its S-protein to the cellular receptor ACE2. The ADE phenomenon can be classified as two different mechanisms: ADE through enhanced infection and ADE through enhanced immune activation. (b) In ADE through increased infection, antibodies of a non-neutralizing or sub-neutralizing nature cause viral infection through FcγRIIa-mediated endocytosis, resulting in a more severe disease phenotype. (c) In ADE via enhanced immune activation, non-neutralizing antibodies can form immune complexes with viral antigens inside airway tissues.
ADE phenomenon. (a) The conventional mechanism of infection by SARS-CoV 2 consists of the binding of its S-protein to the cellular receptor ACE2. The ADE phenomenon can be classified as two different mechanisms: ADE through enhanced infection and ADE through enhanced immune activation. (b) In ADE through increased infection, antibodies of a non-neutralizing or sub-neutralizing nature cause viral infection through FcγRIIa-mediated endocytosis, resulting in a more severe disease phenotype. (c) In ADE via enhanced immune activation, non-neutralizing antibodies can form immune complexes with viral antigens inside airway tissues.
A Closer Look at ADE
Taking a closer look, when humans are exposed to a virus, two types of immune responses occur. The innate immune response is the body's initial, fast-acting, non-specific response to a pathogen. A few days after the innate immune response, the adaptive immune response, which incorporates antibodies, takes over. This response creates a more specific action to fight off the intruder. A primary objective of these antibodies—called neutralizing antibodies—is to bind to the pathogen and prevent it from infecting (or entering) a cell. Neutralizing antibodies can recognize specific proteins unique to a virus (called antigens). This action helps them quickly remember and respond to the pathogen if they're exposed to it again, helping to prevent a potential infection. Many vaccines work by inducing neutralizing antibodies.
As previously mentioned, antibodies are usually helpful in preventing viruses from infecting cells. But sometimes, they can worsen an infection—this is called ADE. ADE occurs when the antibodies generated during an adaptive immune response recognize and bind to a pathogen, but they cannot prevent infection. Instead, these antibodies act as a "Trojan horse," allowing the pathogen to invade cells and multiply, worsening the immune response. Additionally, antibodies can react with viral antigens inside your body, causing inflammation in infected organs.
yLJxDfZYk6HAT-6SjWo8Hg
ADE and Vaccines
Though not automatically evidence of ADE, researchers suggest that when a vaccinated individual becomes infected with the pathogen against which the vaccine is intended to prevent, three different scenarios can occur:
- Mild illness — In this scenario, the person may experience some symptoms, but they are more of an inconvenience and last only a few days (typically about 1-3 days). This is common for many respiratory and gastrointestinal infections (e.g., influenza, COVID-19, and rotavirus). According to experts, these mild symptoms are evidence that the vaccine worked.
- "Breakthrough illness" — Traditionally, this term has been reserved for vaccinated people who get more severely ill, requiring hospitalization or experiencing untoward outcomes, such as disease complications (e.g., pneumonia) or death. In this case, the vaccine may not have worked at all, or it did not induce high enough levels of immunity to effectively stop an infection.
- ADE — In this scenario, the antibodies that the vaccine generated actually help the virus infect more significant numbers of cells than it would have on its own. In this situation, the antibodies bind to the virus and help it more easily get into cells than it would on its own. The result is often more severe illness than if the person had been unvaccinated. ADE can occur after disease and has on occasion been identified following vaccination. As noted by Children's Hospital of Philadelphia, "any vaccine found to cause ADE has stopped being used or, more recently as is the case with the dengue vaccine, has been recommended only for those who will not be affected by ADE. Evidence of ADE has not emerged for COVID-19 vaccines, even though concerns have been raised."
Without question, vaccines have been known to cause ADE. Historically, vaccines have been designed to prevent infections and serious illnesses by imitating an infection. This mechanism triggers an adaptive immune response in the body. After receiving a vaccination, the body produces cells that create antibodies to protect it from future infection. In some rare cases, a vaccine may push the body to make antibodies that don't neutralize the virus, leading to ADE. As explained above, these antibodies can allow the virus to multiply or cause inflammation, making the individual even sicker. The clinical trials were either stopped when this occurred, or the vaccine was withdrawn from the market.
The Ignored Risk of ADE and Mass COVID-19 Vaccination
Though largely ignored by government agencies and experts advising the Biden administration's mass vaccination campaign, multiple reputable scientists and doctors have issued repeated warnings about COVID-19 jabs and ADE. Dr. Robert Malone recently shared his opinion on the latest COVID-19 variant Omicron and mass vaccination and ADE.
Dr. Malone pointed out that with Omicron, "we are truly blessed because it has such a low risk of severe disease and death." However, he added, "it's got a warning sign, and it's what Geert has been warning about. It is [also] what the FDA acknowledged in the original documents allowing the emergency use authorization. [They] told the pharmaceutical industry that they hoped that it would investigate the risks of ADE (or vaccine-enhanced disease)." He continued, warning:
"What Geert has been warning us about, quite stridently, is if we continue to implement this universal vaccination policy—rather than the position of the Great Barrington Declaration—in the face of the pandemic (particularly with Omicron, a much more infectious virus), we risk driving the virus through basic evolution to a state where it may be more pathogenic and more able to allude immune response in some.
If we continue to pursue universal vaccination, the high probability is that we will continue to see the evolution of additional escape mutants that are increasingly infectious and may very well become more pathogenic.
This policy of forced universal vaccination is absolutely contrary to all of our understanding of basic viral evolution. We are clearly seeing the development of escape mutants that are resistant to the vaccine. Omicron is not only resistant to the vaccine, but its infectivity seems to be facilitated by the vaccine. And in my opinion, this must stop for the sake of the world."
KJGuQikfQQ4UqJ2BSxo4lQ
Original Antigenic Sin And Omicron Boosters
With the race by Moderna and Pfizer-BioNTech to develop Omicron-specific boosters, concern around a concept called "original antigenic sin" (OAS) is gaining attention. Similar in potentially negative consequences but different than ADE, in this scenario, the immune system's response is tailored to the first version of the virus, and its responses to subsequent variants are much less effective. With over 50 mutations, Omicron is different enough from previous variants in that antibodies made for the original version of the virus stumble to identify the latest version.
Researchers first discovered OAS when analyzing how older people respond to flu vaccines. With over 20 different flu viruses, different strains are dominant in different years, and each evolves rapidly. Every fall, flu-vaccine manufacturers try to include the proper virus—and the correct version of each of those viruses—in the annual flu shot, hoping to induce antibodies that match the virus people are most likely to encounter.
 Screenshot / Francis, Thomas. "On the Doctrine of Original Antigenic Sin." Proceedings of the American Philosophical Society, vol. 104, no. 6, American Philosophical Society, 1960, pp. 572–78, http://www.jstor.org/stable/985534.
Screenshot / Francis, Thomas. "On the Doctrine of Original Antigenic Sin." Proceedings of the American Philosophical Society, vol. 104, no. 6, American Philosophical Society, 1960, pp. 572–78, http://www.jstor.org/stable/985534.
However, researchers found—regardless of the vaccine's design—individuals produced the best and longest-lived antibodies against the flu strains they were first exposed to as kids. Despite assurances from BioNTech CEO Uğur Şahin that this is not the case with COVID-19 vaccines, boosters, and infections, researchers have expressed concern that OAS may come into play with COVID jabs.
Although vaccine manufacturers declare it's relatively straightforward to design an mRNA vaccine that codes for a new spike protein, it is unclear whether the body's immune system would be nimble enough to adapt to the new instructions. Experts wonder if, when injected with a variant-specific booster, those jabbed would predominantly churn out copies of the antibodies they made after their first vaccination or infection. That scenario would give the world far less latitude to respond to an immune-evasive variant like Omicron. Not concerned about OAS, John Mascola, head of the National Institute of Health's vaccine research center, declared:
"What we've seen suggests that antigenic imprinting … is not going to be a problem. I shouldn't say it's not going to be a problem, but it hasn't been a problem so far."


