The Department of Health and Human Services (HHS) made changes in hospital guidelines for reporting on Jan. 6, which could add to confusion over the interpretation of COVID-19 data for children. Adding multiple entries for pediatric inpatient and ICU beds, the new pediatric reporting requirements could be subject to misinterpretation. The HHS Protect system is apparently also concurrently dropping the requirement that America's hospitals report daily COVID-19 deaths.
Below is a map of participating states from the website.
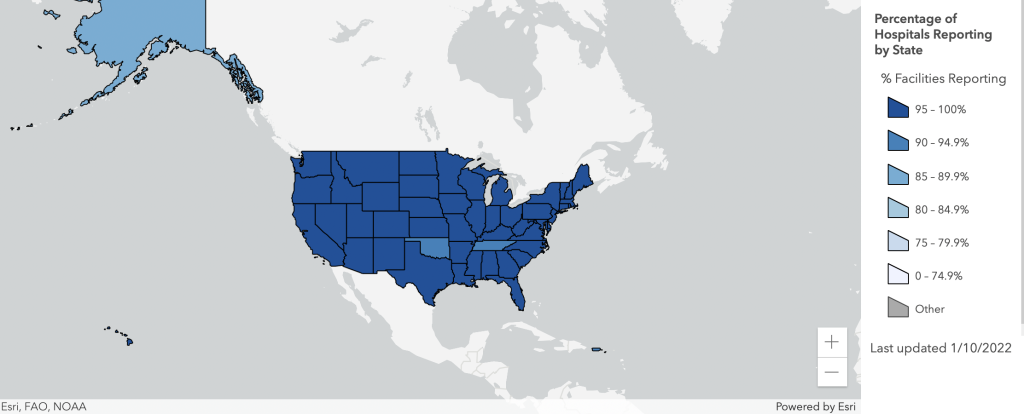 HHS.gov/Hospitals Reporting by State
HHS.gov/Hospitals Reporting by State
This uncoupling of data could drive misinterpretation of data and, therefore, unnecessary worry over the way COVID-19 affects children. HHS requires that the changes be made by Feb. 2, 2022. The Trump administration asked that data be directly reported to HHS in the summer of 2020.
Steve Murch, a Harvard MBA graduate and entrepreneur, states in his Jan. 16 data analysis of the HHS changes, that in the current environment, the new reporting guidelines could easily show up in the media or from officials in the form of unnecessary alarm:
"The net result of these changes is that it is we will likely soon see media reports along the lines of "Pediatric COVID Hospitalizations Rise Alarmingly," and "Pediatric ICU Beds Near Capacity," when the underlying truth is that worrisome COVID among our youngest adults has been, and remains, extremely low — at the level we should worry about seasonal influenza."
A list of the changes and the deadline for the changes in reporting can be found in the Appendix A Change Log beginning on page 26, captured below:
 HHS/Appendix A Change Log
HHS/Appendix A Change Log
Page 27 shows the inactive reporting requirements to include the removal of reporting the previous day's COVID-19 deaths.
 HHS/Inactive Requirements As of Jan. 6
HHS/Inactive Requirements As of Jan. 6
Notably, as an aside, other datapoint removals are also puzzling. Why is HHS dropping data on ventilators and staffing? It is known that those on ventilators due to COVID-19 illness have a higher risk of death. Therefore, HHS is removing another indicator of severe illness that could provide clues about what is going on in hospitals. Staffing in hospitals may be significantly impacted by vaccination status. Why now are staffing data no longer important?
The reporting changes are also highlighted in the Data Element Table shown on pages 6 through 24. The primary driver for the pediatric reporting changes seems to stress the availability of beds for children in hospitals and reporting of laboratory-confirmed COVID-19 in children, as detailed in Appendix B on pages 30 through 38:
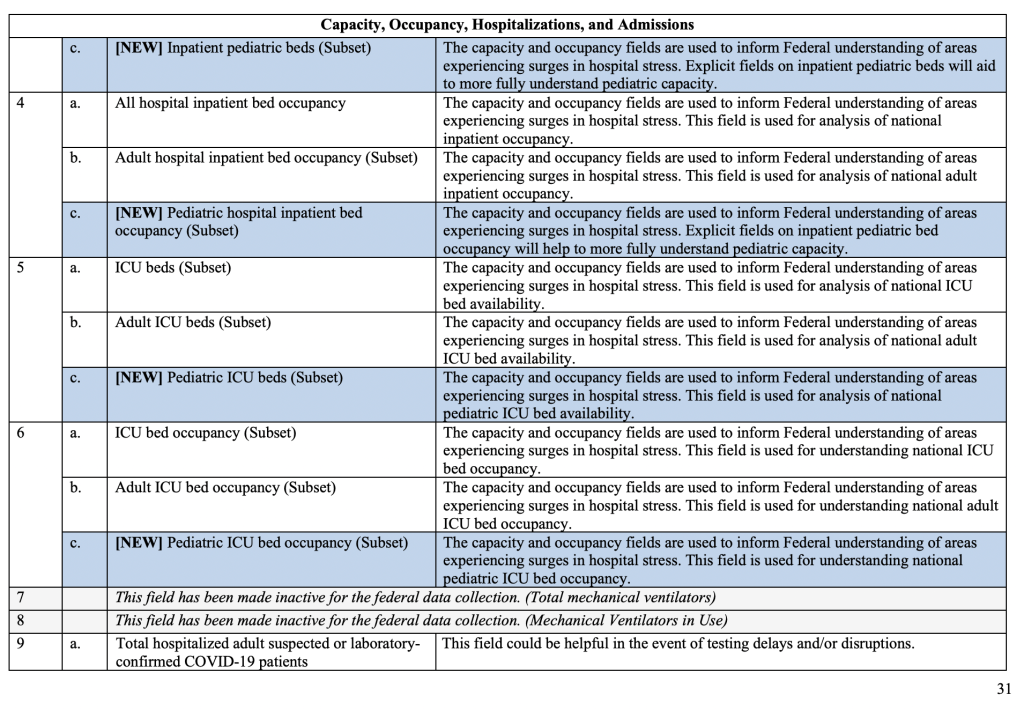
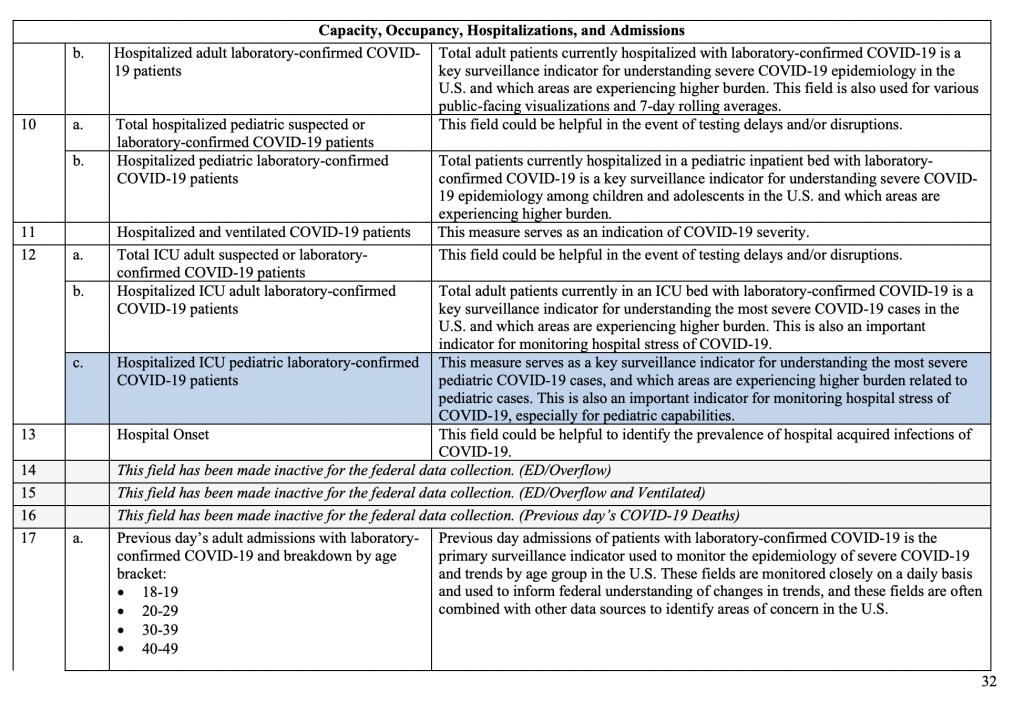
Here, HHS breaks pediatric admissions data into four groups. The reporting looks at laboratory-confirmed COVID-19 cases but doesn't seem to indicate the reasons for hospitalization clearly. In other words, there is no language specifying that a child's hospitalization is directly related to disease from COVID-19. Rather, it seems to stress only "how pediatric admissions compare to adult."
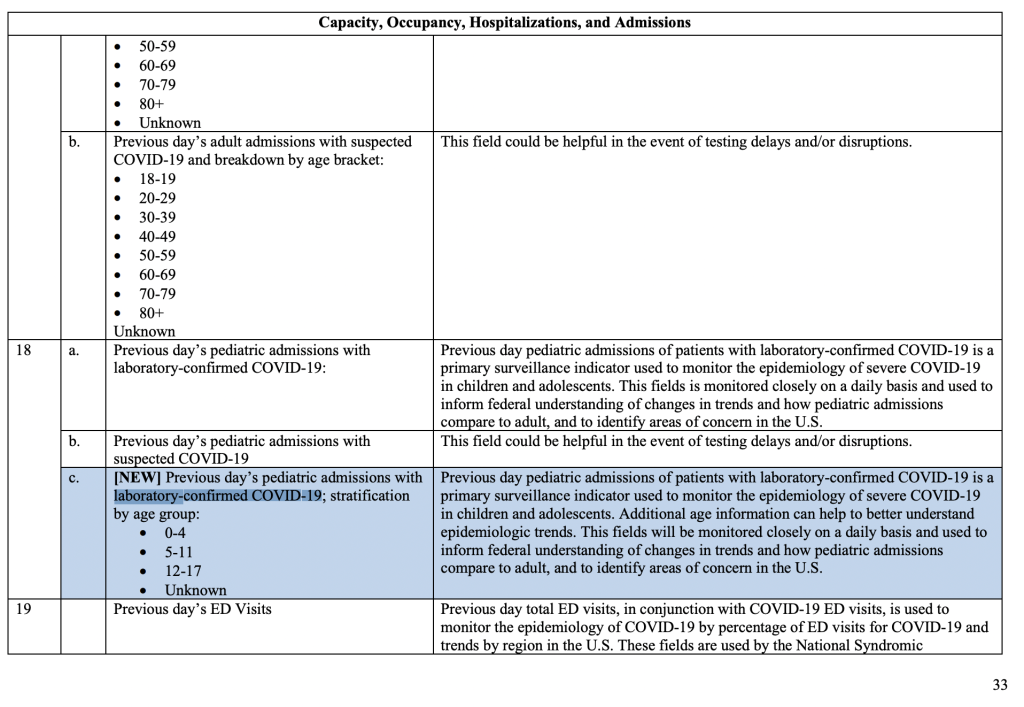 HHS/Appendix B
HHS/Appendix B
It is perplexing to see HHS suddenly adding so many pediatric data points while also dropping the reporting of deaths, especially in the current climate of chaotic government messaging and fear over the virus.
What Does The Data By Age Group Say?
A dispassionate analysis of the data concerning the risk of death from COVID-19 in children is extremely important to keep in mind. Oddly, throughout the pandemic, it has been exceedingly difficult to get COVID-19 data on children to stick in the minds of many Americans.
The data collected on deaths by age group seem to definitively show that the risk of death to children from COVID-19 is very low. The chart below, pictured according to age groups from statista.com, shows that the risk continues to be highest in the elderly, especially those over 75 years in age. And the supplementary notes emphasize that age groups with an * represent groups where the percentage of deaths was less than 0.1 percent. Who are those groups? Children 17 years and younger.
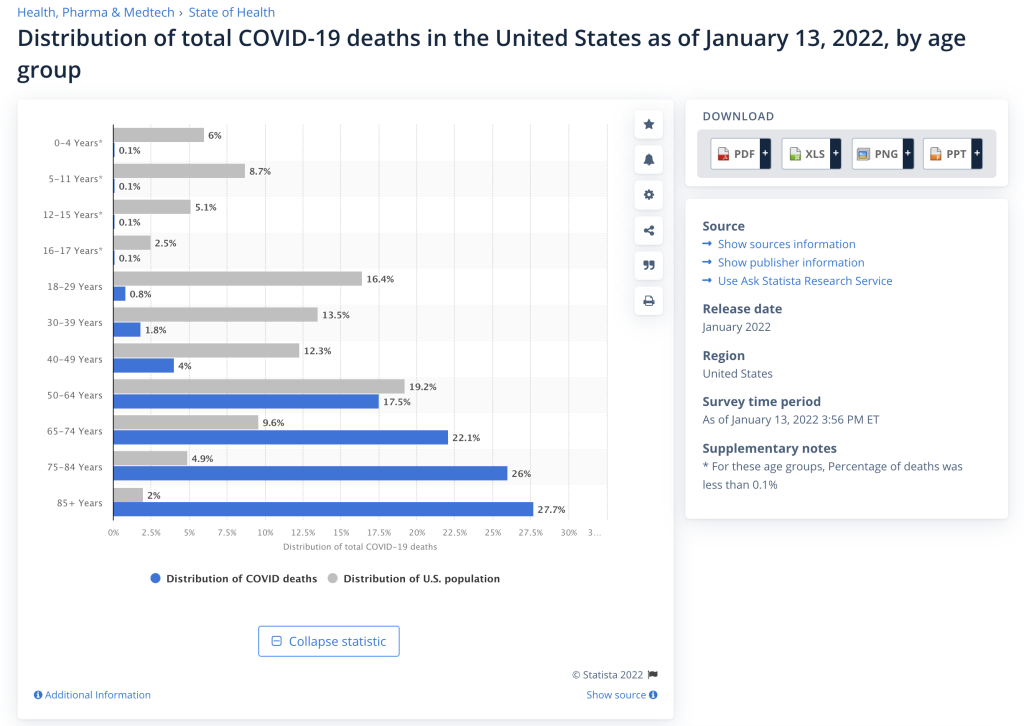 Statista.com/Deaths by Age Group/Jan. 13,2022
Statista.com/Deaths by Age Group/Jan. 13,2022
Murch pulls in data from the NY Times that "visualizes CDC mortality risk" in children comparing causes of death from May of 2021. If the collected data is accurate, COVID-19 is the least likely cause of death in children.
 NYTimes/Causes of Death in Children As Compared to COVID-19
NYTimes/Causes of Death in Children As Compared to COVID-19
Finally, the CDC.gov webpage shows data collected by age group reported to the National Center for Health Statistics (NCHS) on "deaths occurring within the 50 states and the District of Columbia that have been received and coded as of the date specified." A partial capture of the data clearly indicates that the likelihood of a child dying from COVID-19 is still very low.
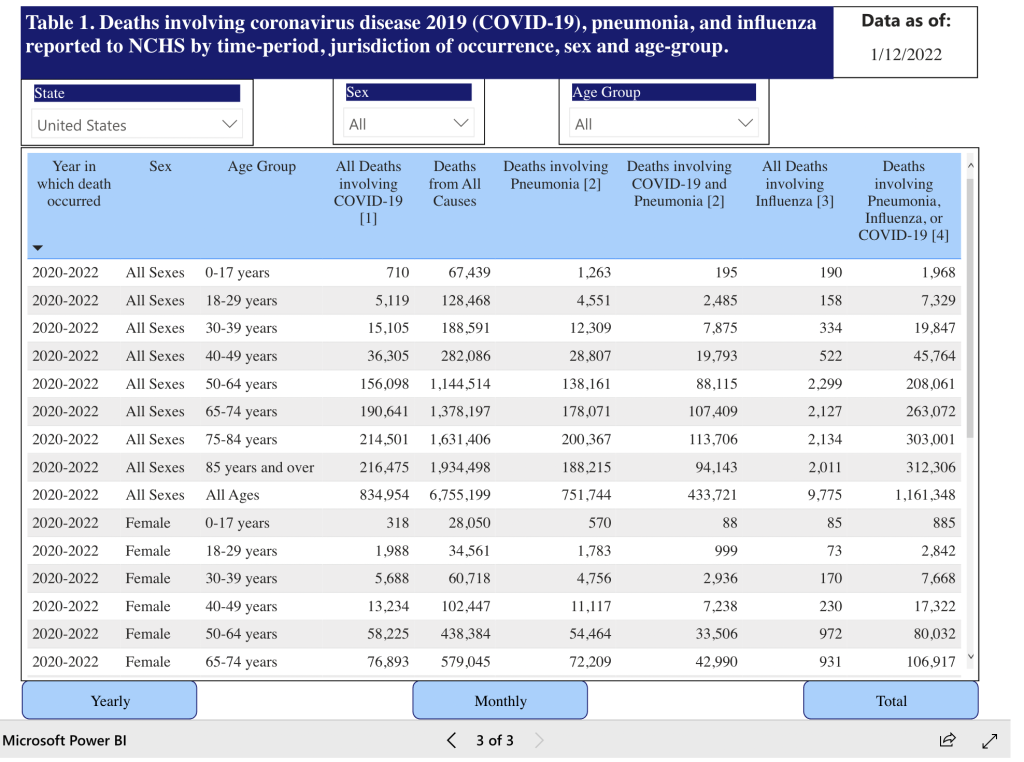 CDC.gov/Deaths in Children Causes
CDC.gov/Deaths in Children Causes
Hospitals all over the country are testing for COVID-19 upon admission. However, a positive COVID-19 test upon admission does not necessarily mean the patient was admitted because of COVID-19 symptoms. Some patients go to the hospital for other reasons, only to find they test positive for the virus.
In light of this kind of testing and the new reporting guidelines, Murch's discussion is worth some proper reflection, especially concerning the data on children:
"But here's how that, plus the new metrics above, clouds the interpretation. Let's say you have 5 ICU beds dedicated to your pediatric wing. A recent icy weekend has caused four of those beds to be occupied: two by kids with broken bones or needing stitches for serious injury, one for a grave car accident, and one who presented for appendicitis. Zero of them presented to the hospital because of COVID, but upon routine testing, four of them are COVID-positive because there's an outbreak in your region at the moment."
"Your accurate reporting to HHS, under these new guidelines, will be that 80% of your pediatric ICU beds were taken up by COVID patients. Sum that same scenario up from thousands of hospitals across the country, and deliver it on a nice-looking dashboard. Journalists from around the country will read the dashboard and rush to their media feeds with accurate but misleading headlines: "80% of Pediatric Beds Taken Up By COVID Patients," or "Alarming Rise in Serious COVID Cases In Young Adults." Infographics will show that pediatric COVID is on the rise (because, at a minimum, hospitals weren't required to break out this data.) Scary infographics will course through social media."
So, what are we to do with HHS reporting that fails to distinguish between death-threatening COVID-19 admissions and those that are incidental COVID-19 admissions? The COVID-19 "with vs. from" distinction in hospital admissions is critical data and should not be obscured. Even Fauci admits it is an important distinction here in December. In early January, Governor Kathy Hochul of New York also made the distinction, saying it is "vital to calming needless fears."
COVID-19 Reporting Has Always Been A Nightmare
The reporting of COVID-19 deaths has always been difficult to parse. Delays in reporting have been an issue from the beginning. Notably, state and local health departments are still reporting death counts to the CDC so that data can be found. Language at the beginning of the HHS announcement explains:
 HHS Opening Statement/Reporting Changes
HHS Opening Statement/Reporting Changes
However, some states, like Florida, seem to be dropping real-time reporting data on deaths and can now no longer rely on HHS for COVID-19 related deaths. So, to understand the data from Florida, one would need to look at inferred data from the CDC to attempt to understand the number of COVID-19 deaths in Florida.
We are sorely in need of consistent, real-time data on COVID-19 if public policy on the matter is to be respected. The changes in reporting are puzzling if transparency is truly a priority. Policies that dictate lockdowns, masks, vaccines, and other draconian measures should be as well-grounded in accurate, real-time data as possible.
Most importantly, we owe it to our children, who have now been subjected to two years of masks, virtual learning, and quarantines, to provide accurate information on their level of risk and/or death. Reporting like this may leave too much room for fear and misinformation.


