Emphasizing the importance of natural immunity, a Swedish study published on Mar. 31, 2022, in The Lancet concludes that if vaccine passports are used for societal restrictions related to COVID-19, they should also recognize a previous infection as proof of immunity instead of focusing only on a person' vaccination status.
As the World Health Organization (WHO) continues to push for an international vaccine "passport," the study, which included over 8.5 million subjects across Sweden, revealed that the risk of SARS-CoV-2 reinfection and COVID-19 hospitalizations for those already infected and recovered remains extremely low for at least up to 20 months. Likewise, the study noted that vaccination seemed to "further decrease the risk of both outcomes for up to 9 months, although the differences in absolute numbers, especially in hospitalizations, were small."
The extensive study was conducted by three Umeå University researchers under the leadership of Prof. Peter Nordstrom, a physician with the Department of Community Medicine and Rehabilitation. The retrospective cohort study created three cohorts using Swedish nationwide records managed by the Public Health Agency of Sweden, the National Board of Health and Welfare, and Statistics Sweden.
Explanation of Study Groups
Cohort 1 included unvaccinated individuals with natural immunity matched pairwise on birth year and sex to unvaccinated individuals without natural immunity at baseline. Cohort 2 and cohort 3 included individuals vaccinated with one dose (one-dose hybrid immunity) or two doses (two-dose hybrid immunity) of a COVID-19 vaccine, respectively, after a previous infection, matched pairwise on birth year and sex to individuals with natural immunity at baseline. Outcomes of the study were documented SARS-CoV-2 infection from Mar. 20, 2020, until Oct. 4, 2021, and inpatient hospitalization with COVID-19 as the primary diagnosis from Mar. 30, 2020, until Sept. 5, 2021. A breakdown of the number of individuals in each Cohort is as follows:
Cohort 1 - Natural Immunity 2,039,106
Cohort 2 - One-dose hybrid immunity 2,962,318
Cohort 3 - Two-dose hybrid immunity 3,567,810
Total 8,569,234

Overview of Results Reinforcing the Relevance of Natural Immunity
At a mean follow-up period of 164 days (SD 100), the team reported 34,090 persons with natural immunity in cohort 1 compared with 99,168 infections in non-immune persons, while the hospitalizations numbers were 3,195 and 1,976, respectively.
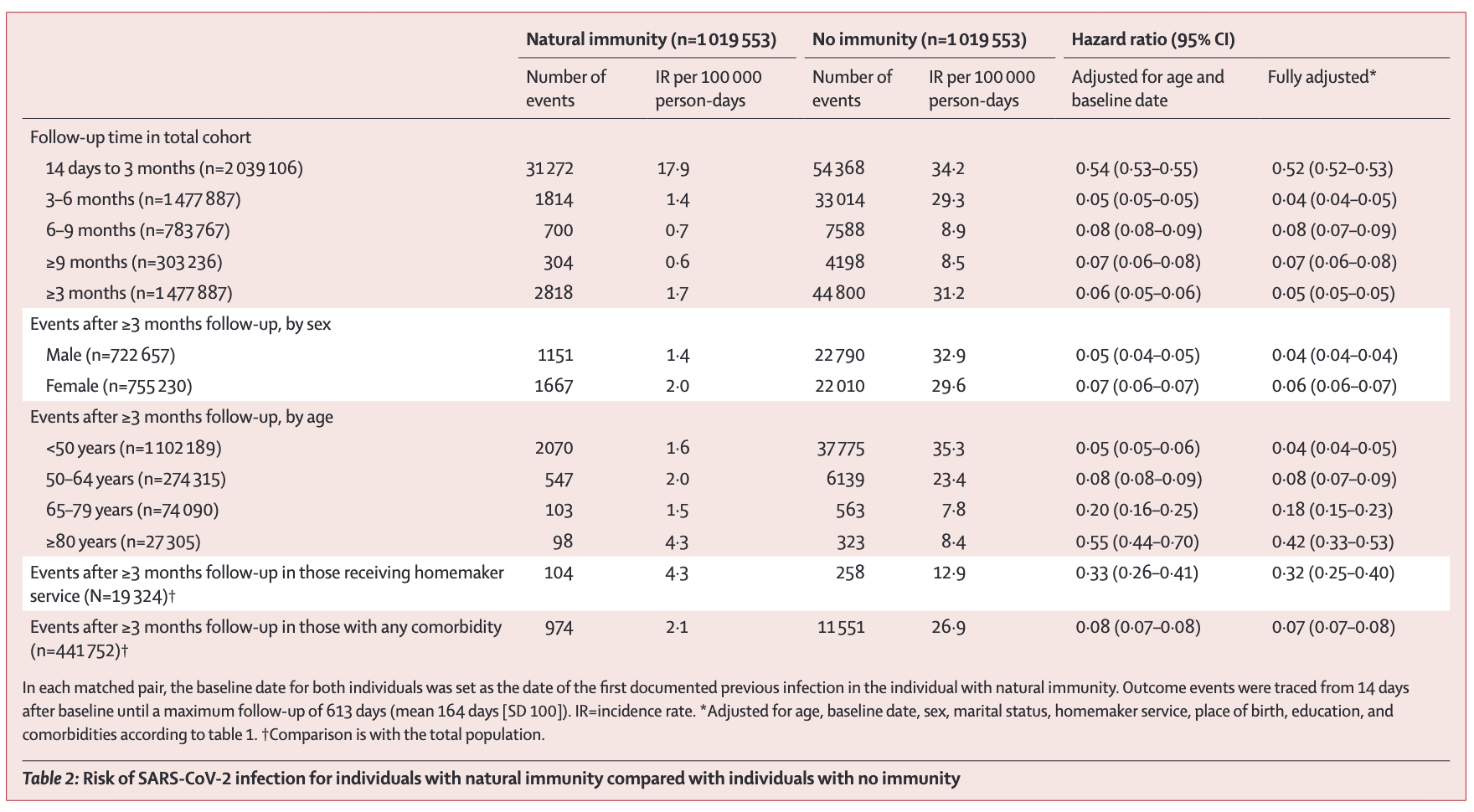
At three months post-infection, natural immunity was associated with a 95 percent lower risk of COVID-19 and an 87 percent lower risk of COVID-19 hospitalization for up to 20 months of medical follow-up. Furthermore, the team recorded that at 52 days of mean follow-up (SD 38) in Cohort 2, 639 subjects with one-dose hybrid immunity were registered with a COVID-19 infection, compared with 162 people with natural immunity (hospitalizations were 8 and 113, respectively).
The researchers documented that one-dose hybrid immunity was associated with a 58 percent lower risk of COVID-19 reinfection than natural immunity up to the first two months, with evidence of attenuation after that up to 9 months of follow-up. At a follow-up of 66 days (SD 53), when delving into cohort 3, the study team reported 438 subjects with two-dose hybrid immunity registered COVID-19 reinfection compared to 808 subjects with natural immunity (hospitalization numbers included 6 and 40, respectively).
Conclusion
The researchers noted that many government health experts recommend that all individuals receive both the first and second COVID-19 vaccine and boosters regardless of whether they've previously been infected. However, they also pointed out that the strongest argument behind this recommendation "might be the scarcity of evidence on long-term protection from natural immunity."
Their study expands the body of evidence on the power of natural immunity with up to 20 months of follow-up and more than 130,000 documented SARS-CoV-2 infections. The results established that individuals with natural immunity had an associated 95 percent protection against SARS-CoV-2 reinfection during follow-up—from 3 months after initial infection until 20 months—with no signs of waning. The results indicate that natural immunity might be better sustained than immunity induced by COVID-19 vaccination only, as also suggested by initial data from an Israeli study.
In further support of the researcher's findings (the complete study can be found here), they recently reported waning vaccine effectiveness against SARS-CoV-2 infection within a few months in a similar study based on the total population of Sweden. Another important finding of the current study is the connection between natural immunity and later hospitalization for reinfection, which has not previously been reported in the literature. The authors explained:
"As expected, there was an increased risk of hospitalization during the first 3 months after the first infection, but for those who survived, natural immunity was associated with 87% protection against COVID-19 hospitalization during the rest of follow-up. The associated level of protection remained high (78%) even from 9 up to 19 months of follow-up, altogether indicating long-lasting protection, including against severe disease, from natural immunity. Together, these findings might suggest that any passports or documents used to identify whether a person is immune or not, and used for societal restrictions, should acknowledge either a previous infection or vaccination as proof of immunity, as opposed to vaccination only. This policy could have social and equity implications, especially for individuals in countries with low vaccine coverage, considering also that the dominant omicron variant is less sensitive to current vaccines than previous variants."


